Shingles Vs Cold Sores
The viruses that cause shingles and cold sores are in the same family, herpesviridae, but are different species. Cold sores are generally caused by herpes simplex virus-1 while shingles is caused by the varicella-zoster virus .
While there are two vaccines available to prevent shingles outbreaks, their protection does not carry over to the herpes virus that causes cold sores . There are no vaccines available to prevent infection or outbreak of HSV-1.
Cases Of Herpes Zoster Infections Following Covid
One of the earliest reports of herpes zoster infection post COVID-19 vaccination was published in April 2021 in the journal Rheumatology. The study analyzed side effect data from 491 people with autoimmune inflammatory rheumatic diseases who received the Pfizer-BioNTech vaccine.
The researchers found that six of the patients with AIIRD developed herpes zosteraka shingleswithin several days of receiving the vaccine. Four of the patients had rheumatoid arthritis, one had Sjogren’s syndrome, and another had a connective disease. All of the patients were women, and five of the reactions happened after the first vaccine dose.
The herpes zoster infection was mild in the majority of cases, although one patient had a case of herpes zoster ophthalmicus, which is when the virus impacts the eye. Five of the patients were treated with antiviral medication and had no symptoms up to six weeks later. Five of the patients completed their second dose of the vaccine without any other issues.
In February 2022, a study published in the British Journal of Clinical Pharmacology looked at the relative risk of HZ reporting in mRNA COVID-19 vaccine recipients compared to influenza vaccine recipients. Researchers used the database VigiBase, the World Health Organization global database which contains about 27 million spontaneous reports of suspected adverse drug reactions collected by national drug authorities in more than 130 countries.
What Are The Symptoms Of Herpes Zoster
At first, people with shingles may have a burning, itching, numb, or tingling pain that can be severe, NINDS says. It usually happens on one side of the body. People develop shingles after they’ve had a previous chickenpox exposure. When the virus reactivates, it causes shingles.
After a few days, a rash of fluid-filled blisters will appear in one area on one side of the body, NINDS explains. Shingles most commonly shows up in a band called a dermatome that goes from one side of your midsection around your waistline.
The pain from shingles can varysome people mostly itch Others can have pain from a gentle touch.
Recommended Reading: Does Csl Plasma Test For Herpes
Can The Shingles Vaccine Cause A Genital Herpes Outbreak
Question posted by artsyrsc on 13 Nov 2014
Last updated on 22 August 2022 by ResaW
I got my vaccine on a Friday, felt headachy and rundown all weekend. By Tuesday I was getting an outbreak. I hadn’t had one in a pretty long time and I take acyclovir when I do. Coincidence or a side effect of the vaccine?
ResaW
I have had oral Herpes for ages, but I was fastidious about not infecting my genitals and for decades thought I had succeeded.
After the 2nd shot of Shingrix I developed genital herpes :-/
These outbreaks are more common than they ever were on my mouth and I’m sad.
Not saying correlation means causation by any means, but I thought I should add this bit of anecdotal evidence for this question.
+0Snowy-8Sugar13
I am 50, diagnosed with HSV2 thru blood work a few years ago, but never had an outbreak before. I got 2nd Shingrix a couple of weeks ago. Arm pain and body aches with fatigue for a couple of daysthen a genital outbreak. I had no clue what it was since Ive never had an outbreak before. Luckily it was small and minimal pain. Coincidence? I didnt think so until I read here.
+1jaxonp+1Em6638
Something happened to me a herpes outbreak after the Shingles Vaccine. I Had not had outbreak in 15 yrs.
+1Salsify+0SEM42SalsifySEM42
for anyone reading this: if you get a strong vaccine , TAKE VALACYCLOVIR AT THE TIME YOU GET THE VACCINE, A HIGH DOSE LIKE 2 GM. and keep taking it for about 2 days. this should help block any reactivation. I wish I had known.
+1+1
Approaches To Vaccine Development

Although there are no currently available vaccines for herpes simplex 1 and 2, there are various candidates in both the pre-clinical and the clinical phases currently in development. Vaccines are being developed with two broad focuses: preventative and therapeutic, some with a dual use. Preventative vaccines are focused on the prevention of primary infection in a seronegative subject. Therapeutic vaccines aim to prevent HSV reactivation, decrease the number of recurrences, or to reduce the severity or duration of clinical symptoms . With regard to vaccine development, given our knowledge of the immunology surrounding HSV, it seems that an effective vaccine would likely stimulate not only humoral responses, but also cell-mediated responses. Different vaccine subtypes have their unique advantages and disadvantages, discussed further in the next section.
Recombinant vaccines are usually composed of proteins that are not strong immunoactivators. Therefore, they require adjuvants to stimulate the innate immune system. This leads to the humoral response and proper inoculation. They are not needed for live-attenuated viruses. Different constituents can enhance and target different facets of the immune response. It is important to focus on the adjuvants in each vaccine trial and evaluate their role in eliciting a lasting humoral and cell-mediated response .
Don’t Miss: What To Do If I Think I Have Herpes
What Should You Expect If You Get Shingles
Shingles can be a very painful condition. If you think you have the symptoms of shingles, see your healthcare provider right away. Starting antiviral medications early can ease your discomfort and end symptoms earlier.
A better approach to shingles is to take action and do what you can to lessen your risk of getting it. If you’ve never had shingles in the past, talk to your healthcare provider about getting the shingles vaccine. If youve never had chickenpox, talk with your healthcare provider about getting the chickenpox vaccine.
Is A Vaccine Available To Prevent Shingles
Two vaccines are available in the United States to reduce your chance of developing shingles and postherpetic neuralgia. One vaccine, Zostavax®, has been available since 2006. The second vaccine, Shingrix®, has been available since 2017. Shingrix is recommended as the preferred vaccine by the Advisory Committee on Immunization Practices, a group of medical and public health experts.
Shingrix is given as a two-dose shot in your upper arm. You should receive the second dose two to six months after receiving the first. Shingrix has been shown to be more than 90% effective in preventing shingles and postherpetic neuralgia. Its effectiveness remains above 85% for at least four years after receiving the vaccine.
Don’t Miss: How To Treat Herpes Type 1
Is Chickenpox And Shingles A Form Of Herpes
Though shingles and herpes are two distinct conditions caused by two distinct viruses, the viruses are both members of a family formally known as herpesviridae. The herpes simplex virus takes its formal name from this umbrella term, while the varicella-zoster virus does not.
Although it is a condition unrelated to herpes, shingles is sometimes referred to as herpes zoster, a nickname that references the shared family of the viruses that cause them. Within this viral family, only the herpes simplex virus causes the condition we know today as herpes.
If you are ever unsure whether your doctor is referring to herpes simplex or shingles when you hear the word herpes, ask for clarification.
If You Get The Shingles Vaccine Does This Mean Youre 100% Protected From Getting Shingles
No. Just like most vaccines, getting vaccinated with a shingles vaccine doesnt provide 100% protection from disease. However, getting the shingles vaccine reduces your risk of developing shingles.
Even if you do develop shingles, youll be more likely to have a mild case. Also, youll be much less likely to develop postherpetic neuralgia, a painful condition that can follow a shingles outbreak.
Recommended Reading: What Are The Chances Of Getting Herpes
How Cdc Monitors Vaccine Safety
CDC and FDA monitor the safety of vaccines after they are approved or authorized. If a problem is found with a vaccine, CDC and FDA will inform health officials, health care providers, and the public.
CDC uses 3 systems to monitor vaccine safety:
- The Vaccine Adverse Event Reporting System : an early warning system, co-managed by CDC and FDA, to monitor for potential vaccine safety problems. Anyone can report possible vaccine side effects to VAERS.
- The Vaccine Safety Datalink : a collaboration between CDC and 9 health care organizations that conducts vaccine safety monitoring and research.
- The Clinical Immunization Safety Assessment Project: a partnership between CDC and several medical research centers that provides expert consultation and conducts clinical research on vaccine-associated health risks.
Is There Any Resistance To Genital Herpes Medication
Resistance to drugs that treat genital herpes even after 20 years of use is very rare. Herpes medications may not work as well in patients who are very immunosuppressed and have been treated with these drugs for a long time. Each individuals response to treatment may vary. In some cases, patients may need more drugs to suppress their viral outbreaks than others.
You May Like: How To Get Tested For Oral Herpes
Who Should Not Be Vaccinated With Shingrix
You shouldnt receive the Shingrix vaccine if you:
- Have ever had a severe allergy to this vaccine or any ingredient in this vaccine.
- Are breastfeeding or pregnant.
- Currently have shingles.
- Are ill and have a high fever.
- Have tested negative for immunity to varicella-zoster virus .
Ask your healthcare provider if the benefits of getting the vaccine outweigh any potential risks.
About Author: David Pruitt

David Pruitt is a writer for the Marketing & Communications division of OSF HealthCare. He has a bachelors of journalism from Southern Illinois University Edwardsville and worked as a reporter before joining OSF HealthCare in 2014. An avid golfer and fisherman, David was born and raised Alton, Illinois, which is where he currently resides with his son, James.
Also Check: How Long Does Herpes First Outbreak Last
Clinical Herpes Simplex Infection
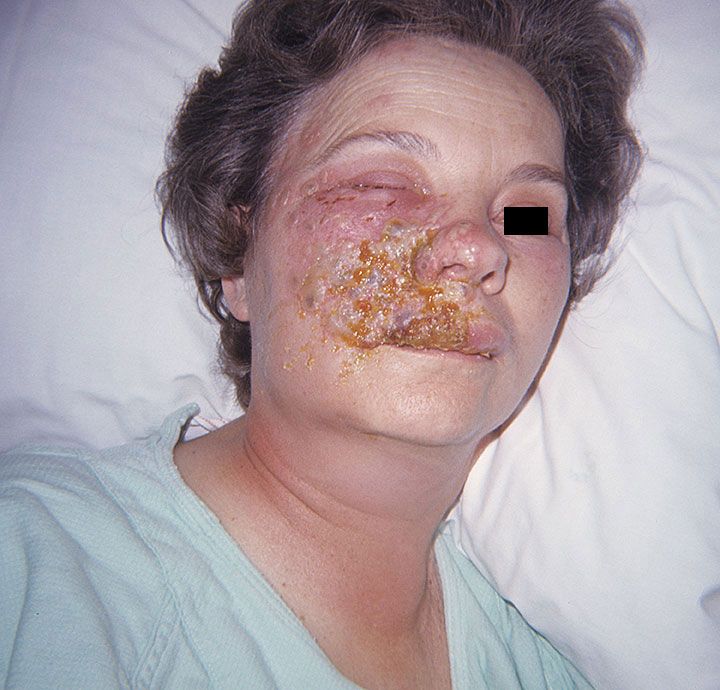
Primary infection with herpes simplex involves grouped vesicles on an erythematous base. Mucocutaneus manifestations include eczema herpeticum, herpetic whitlow, herpes gladiatorum, folliculitis, or a severe/chronic mucocutaneous infection. Extracutaneous manifestations include ocular HSV keratoconjunctivitis. Herpes Encephalitis, Proctitis, and Neonatal HSV. These manifestations are often the ones with prominent morbidity and mortality .
Ocular HSV infection has complications that include corneal ulceration and scarring, globe rupture, and subsequent blindness. Epithelial keratitis has strong links to viral replication, while stromal keratitis is primarily immunopathologic and is promoted mainly by T cells . Consequently, HSV is one of the main causes of infectious blindness in developed countries .
Herpes encephalitis has > 70% mortality without treatment, with residual neurological defects in most surviving patients . Similarly, disseminated neonatal HSV has 50% mortality without treatment, 15% with treatment and with neurologic deficits in many recovering patients .
Further Considerations For The Future Of Herpes Simplex Virus Vaccine Development
Our understanding of the complexities of herpes simplex virus pathogenesis and immune evasion is consistently evolving, along with our understanding of viral latency. Designing an effective therapeutic or prophylactic vaccine requires further understanding these processes.
Trials that had been successful in the pre-clinical realm with murine model and guinea pig models have been effective, but have not translated well in the clinical realm. Other trials like the GSK gD subunit vaccine and the GEN-003 vaccine have been suspended due to dwindling financial support . To us, the HSV-529 and G103 appear to be promising from early studies in the pre-clinical stage. Additionally, they are likely to have less issues with safety as they are not live-attenuated vaccines.
The rapid development of an mRNA vaccine for COVID-19 has re-vitalized interest in mRNA vaccines as viable options to produce viral immunity. The classical problems involving the creation of mRNA vaccines include mRNA stability and delivery systems. It remains to be seen whether mRNA vaccines might have a utility for HSV however, initial studies with the trivalent vaccine have been promising, showing increased efficacy compared to a subunit formulation .
The advantages of an mRNA vaccine were previously discussed: It does not integrate within the host genome, translates in both proliferating and non-proliferating cells, with immediate protein production for a controllable amount of time .
Don’t Miss: How To Prevent Recurrent Herpes Outbreak
When Should I See A Doctor Because Of The Side Effects I Experience From Shingrix
Shingrix causes a strong response in your immune system, so it may produce short-term side effects. These side effects can be uncomfortable, but they are expected and usually go away on their own in 2 or 3 days. You may choose to take over-the-counter pain medicine such as ibuprofen or acetaminophen. Contact your healthcare provider if the symptoms are not improving or if they are getting worse.
In clinical trials, Shingrix was not associated with serious adverse events. In fact, serious side effects from vaccines are extremely rare. For example, for every 1 million doses of a vaccine given, only one or two people might have a severe allergic reaction. Signs of an allergic reaction happen within minutes or hours after vaccination and include hives, swelling of the face and throat, difficulty breathing, a fast heartbeat, dizziness, or weakness. If you experience these or any other life-threatening symptoms, see a doctor right away.
Can You Still Develop Shingles If Youve Been Vaccinated For Chickenpox
Yes. Despite being vaccinated for chickenpox, you can still get shingles. No vaccine is 100% protective, and the effectiveness of vaccines lessens with time. However, people who get the chickenpox vaccine are significantly less likely to develop shingles later in life compared with people who never received the chickenpox vaccine. One recent 12-year study found that the number of shingles cases was 72% lower in children who had received the chickenpox vaccine compared with those who didnt.
Read Also: How To Clear Genital Herpes
Routine Vaccination Of People 50 Years Old And Older
CDC recommends Shingrix for the prevention of herpes zoster and related complications. CDC recommends two doses of Shingrix separated by 2 to 6 months for immunocompetent adults aged 50 years and older:
- Whether or not they report a prior episode of herpes zoster.
- Whether or not they report a prior dose of Zostavax, a shingles vaccine that is no longer available for use in the United States.
- It is not necessary to screen, either verbally or by laboratory serology, for evidence of prior varicella.
Recombinant and adjuvanted vaccines, such as Shingrix, can be administered concomitantly, at different anatomic sites, with other adult vaccines, including COVID-19 vaccines. Coadministration of RZV with adjuvanted influenza vaccine and COVID-19 vaccines is being studied.
Herpes Zoster Vs Herpes Simplex
Herpes zoster is another name for shingles. It’s a viral infection that usually appears as a painful red skin rash and can cause nerve damage and longer-term burning and pain if left untreated. It occurs as a result of the varicella-zoster virus, the virus that causes chickenpox, according to the Mayo Clinic. The first time you’re infected with the virus, it presents as chicken pox on subsequent reactivations, it’s considered herpes zoster or shingles , even though it’s the same virus.
The HZ/shingles rash can develop anytime after you’ve been previously exposed to the virus. If you were born before the advent of the chickenpox vaccine in 1995, you may have had it as a child, and the virus is now lying dormant in your system meaning, it can “reactivate” at any time, and result in HZ/shingles symptoms. If you’re vaccinated against chickenpox and more than 90 percent of U.S. children are currently, according to National Immunization Survey data you can still get shingles later on in life, since the chickenpox vaccine contains small, weakened amounts of the varicella virus. That said, it’s not super common, as Anne A. Gershon, a professor of pediatric infectious disease at Columbia University, explained to Scientific American. “The virus has been altered so the vaccine rarely causes symptoms, but once you’ve been immunized and after the natural infection, you carry the virus in your neurons for the rest of your life,” she said.
Don’t Miss: What Medication Do You Take For Genital Herpes
Improving Our Immune Response To Control Herpes
T cells embedded in tissues where latent HSV-2 hides are known to play a role in controlling the virus. Hutch scientists are also exploring how B cells, the antibody-making factories of the immune system, also work to keep the virus in check. Hutch researchers hope to build on this understanding to develop immunotherapies to control reactivation, reduce transmission to sexual partners, and design vaccines to prevent infection.
What You Need To Know
- Herpes simplex virus , also known as genital herpes, is most likely to be spread when an infected person is having an outbreak, but it can also be transmitted without any symptoms being present.
- Medications can help reduce your symptoms, speed up the healing of an outbreak and make you less contagious.
- If you know you have genital herpes before becoming pregnant, your physician will monitor your condition throughout your pregnancy. If you have an active outbreak at the time of delivery, cesarean section may be recommended.
Don’t Miss: Medication To Prevent Spreading Herpes
What Are The Possible Side Effects Of Shingrix
Studies show that Shingrix is safe. The vaccine helps your body create a strong defense against shingles. As a result, you are likely to have temporary side effects from getting the shots. The side effects might affect your ability to do normal daily activities for 2 to 3 days.
Most people got a sore arm with mild or moderate pain after getting Shingrix, and some also had redness and swelling where they got the shot. Some people felt tired, had muscle pain, a headache, shivering, fever, stomach pain, or nausea. Some people who got Shingrix experienced side effects that prevented them from doing regular activities. Symptoms went away on their own in about 2 to 3 days. Side effects were more common in younger people.
You might have a reaction to the first or second dose of Shingrix, or both doses. If you experience side effects, you may choose to take over-the-counter pain medicine such as ibuprofen or acetaminophen.
Guillain-Barré syndrome , a serious nervous system disorder, has been reported very rarely after Shingrix. There is also a very small increased risk of GBS after having shingles.
If you experience side effects from Shingrix, you should report them to the Vaccine Adverse Event Reporting System . Your doctor might file this report, or you can do it yourself through the VAERS websiteexternal icon, or by calling 1-800-822-7967.
If you have any questions about side effects from Shingrix, talk with your doctor.