How Is Postherpetic Neuralgia Treated
Treatments include lotions or creams and/or other medications not specifically used for pain, such as antidepressants or drugs for epilepsy. Regular pain relievers are not usually effective for this type of pain.
If your pain doesnt lessen, you might try therapies like nerve blocks or steroid injections near the area where the nerves exit the spine. Your provider might suggest an implantable nerve stimulator device for severe, ongoing pain that hasnt responded to other treatments.
Vaccination Of Immunocompromised Adults 19 Years And Older
CDC recommends two doses of RZV for the prevention of shingles and related complications in adults aged 19 years who are or will be immunodeficient or immunosuppressed because of disease or therapy. The second dose of RZV should typically be given 26 months after the first. However, for persons who are or will be immunodeficient or immunosuppressed and who would benefit from completing the series in a shorter period, the second dose can be administered 12 months after the first. For more detailed clinical guidance see .
The Female Factor: Shingles In Women
But, as it turns out, shingles is worse for women across the board. Studies , show that women are at higher risk for the disease and some of its complications, comprising up to about 60% of all cases.
Plus, other research indicates there may be further sex-linked woes for women who get shingles. A Toronto-based study found that females with shingles experienced more hospitalization and outpatient visits, while a Swedish study marked similar patterns. A study from the Mayo Clinic pointed to a higher rate of herpes zoster recurrence in womenrecurrence being the worlds worst threequel and a German study found women experienced higher levels of pain from the disease.
Higher incidence in general, higher risk of recurrence, possibly more pain, and more medical needswhats going on here? Is menopause to blame?
Currently, experts hasten to point out that while the age of 50 absolutely signals the beginning of a spike in shingles risk, there is not yet any significant science to connect the hormonal changes at work at that time directly to the bodys chemistry that allows the virus to reemerge.
We dont know if there are pathophysiological causes in gender differences, says Marla Shapiro, M.D., former president of the North American Menopause Society and a professor in family and community medicine at the University of Toronto. As if to underscore it, she says it again: We just dont know.
Recommended Reading: Can You Be Born With Herpes
You May Like: How To Know If It’s Herpes
Approach To Herpes Simplex Virus Therapy
Nucleoside analogs, including acyclovir, valacyclovir, and famciclovir, remain standard therapies for mucocutaneous and visceral HSV infection. Idoxuridine, trifluorothymidine, vidarabine, and cidofovir are used topically for ocular HSV infections .
Development of HSV resistance to acyclovir and valacyclovir is rare despite extensive use for treatment of infection . Increased prevalence is seen in patients with herpetic keratitis . Antiviral resistance is increased in immunocompromised patients, specifically patients with HIV infections and bone marrow transplants . IV Foscarnet and cidofovir are usually effective for acyclovir resistant viral strains . Continued exposure to cidofovir does not easily induce resistance. However, there have been case reports of cidofovir-resistant HSV and CMV .
Do You Need To Stay Away From Children People Who Are Pregnant Have Cancer Or Anyone With A Weak Immune System After You Get The Zostavax Vaccine

According to the CDC, its safe to be around babies and young children, pregnant women or anyone with a weakened immune system after you get the Zostavax vaccine. Even though the Zostavax vaccine contains a weakened live varicella-zoster virus, the CDC says theres no documented case of a person getting chickenpox from someone who has received the Zostavax vaccine. And remember: You cant get shingles unless youve already had chickenpox.
Read Also: Dr Sebi Curr For Herpes
What Causes Postherpetic Neuralgia
Postherpetic neuralgia results from damage to nerve fibers during shingles infection. The nerve fibers at the skin in the affected area send exaggerated pain signals to your brain. Postherpetic neuralgia means nerve pain after herpes. Shingles is also called herpes zoster.
Shingles is caused by the varicella-zoster virus, the virus that causes chickenpox. Once youve had chickenpox, the virus remains in your body for your entire life, but is dormant or silent for years. When the virus becomes reactivated, it causes shingles. A certain percentage of people who get shingles develop PHN.
Can You Get Shingles From The Covid
There have been a few reports of shingles happening in people who were vaccinated against COVID-19. The varicella-zoster virus was reactivated in these people.
A note from Cleveland Clinic
If youve had chickenpox, youre at risk of developing shingles later in life. Shingles causes a rash that is contagious and painful. The disease can have serious complications. The best thing you can do to reduce your risk is to get the shingles vaccine. The vaccines are safe and effective.
Recommended Reading: Can You Get Pregnant With Herpes 2
What Happens At A Sexual Health Clinic
The doctor or nurse at the sexual health clinic will:
- ask about your symptoms and your sexual partners
- use a small cotton bud to take some fluid from 1 of your blisters or sores for testing
The test cannot:
- be done if you do not have visible blisters or sores
- tell you how long you have had herpes or who you got it from
Symptoms might not appear for weeks or even years after youre infected with the herpes virus.
Dont Miss: Can I Use Abreva For Genital Herpes
Summary And Quick Facts For Herpes And Shingles
- Herpes and shingles are both caused by members of the Herpesviridae family of viruses, which can establish latent infections that remain dormant before reactivating at a later time under certain conditions. Herpes simplex virus-1 and herpes simplex virus-2 cause oral and genital herpes, and varicella-zoster virus causes chickenpox in children and shingles later in life.
- In this protocol, you will learn about the viruses that cause herpes and shingles, and how these infections are conventionally treated. Several natural ingredients that may help ease the symptoms of herpes and shingles will also be discussed, and important lifestyle and dietary considerations that can help prevent outbreaks will be examined as well.
- Antiviral medication is the standard treatment for both shingles and herpes. Although there is no effective cure for herpes virus infections, several natural interventions may help reduce the frequency of outbreaks.
Herpes and shingles are both caused by members of the Herpesviridae family of viruses, which can establish latent infections that remain dormant and then reactivate under certain conditions. Herpes simplex virus-1 and herpes simplex virus-2 cause oral and genital herpes, and varicella-zoster virus causes chickenpox in children and shingles later in life.
Recommended Reading: Is Vitamin C Good For Herpes
Herpes Virus Vaccine Shows Promise In Preclinical Study
A genetically edited form of a herpes simplex virus has outperformed a leading vaccine candidate in a new preclinical study by researchers at the University of Cincinnati, Northwestern University, and the University of Nebraska-Lincoln. The vaccine, called R2, is a form of the herpes simplex virus type 1 virus that causes cold sores around the lip, but can cross-protect against HSV type 2 , the sexually transmitted type of HSV that is usually responsible for genital herpes. To generate the vaccine, the virus was effectively engineered to keep it from taking refuge in the nervous system and eluding an immune response.
The newly reported study showed that vaccinating guinea pigs using the modified live virus vaccine significantly increased the production of virus-combating antibodies. And when challenged with a virulent strain of HSV-2, vaccinated animals displayed fewer genital lesions, reduced viral replication, and less of the viral shedding that spreads infection to others.
The development of an effective vaccine for HSV is a priority because it is a common infection that causes physical and emotional stress as well as increasing the risk for HIV infection, the team noted. The recent failure of subunit HSV vaccines has highlighted the need for vaccines that present a diverse array of antigens, including the development of next-generation live-attenuated vaccines.
Shingles Vaccine: Best Defense Against An Outbreak
About one out of every three people in the United States will develop shingles in their lifetime. Fortunately, the shingles vaccine is a safe and effective way to prevent an outbreak.
If youve had a shingles attack, then you know how painful it can be. However, a shingles attack can have more consequences than just a painful, blistering rash. One of the main complications that can result from a shingles outbreak is postherpetic neuralgia .
PHN causes continuous, chronic pain that lasts even after the skin sores have healed, said Jason Scheid, director of ambulatory pharmacy for OSF HealthCare. It is long-term nerve pain after the rash resolves and can be severe enough to impact your daily life.
Shingles and PHN can be debilitating. Prevention is your best approach.
The older you are when you get shingles, the greater the risk for PHN, Jason said. If the rash presents on your face, there is also a risk of impacting your eye and causing vision problems or even vision loss, so it is essential to be evaluated right away. There is also the potential for rashes and open lesions to become infected.
You May Like: How Soon After Exposure To Herpes Can You Get Tested
Conventional Treatment And Prevention
Standard treatment for herpes virus infections is antiviral medication. The main antiviral medications used for both shingles and herpes are acyclovir, famciclovir , and valacyclovir .10,64,72 All three medications can be taken orally, reduce pain, and speed healing of the lesions however, famciclovir and valacyclovir areoften preferred because they require less frequent dosing than acyclovir.72
Approaches To Vaccine Development
Although there are no currently available vaccines for herpes simplex 1 and 2, there are various candidates in both the pre-clinical and the clinical phases currently in development. Vaccines are being developed with two broad focuses: preventative and therapeutic, some with a dual use. Preventative vaccines are focused on the prevention of primary infection in a seronegative subject. Therapeutic vaccines aim to prevent HSV reactivation, decrease the number of recurrences, or to reduce the severity or duration of clinical symptoms . With regard to vaccine development, given our knowledge of the immunology surrounding HSV, it seems that an effective vaccine would likely stimulate not only humoral responses, but also cell-mediated responses. Different vaccine subtypes have their unique advantages and disadvantages, discussed further in the next section.
Recombinant vaccines are usually composed of proteins that are not strong immunoactivators. Therefore, they require adjuvants to stimulate the innate immune system. This leads to the humoral response and proper inoculation. They are not needed for live-attenuated viruses. Different constituents can enhance and target different facets of the immune response. It is important to focus on the adjuvants in each vaccine trial and evaluate their role in eliciting a lasting humoral and cell-mediated response .
Don’t Miss: Olive Leaf Extract Herpes Cure
For Patients Who Do Not Report A Prior Episode Of Varicella
When vaccinating immunocompetent adults aged 50 years and older, there is no need to screen for a history of varicella or to conduct laboratory testing for serologic evidence of prior varicella. More than 99% of adults aged 50 years and older worldwide have been exposed to varicella-zoster virus, and the Advisory Committee on Immunization Practices considers people born in the United States prior to 1980 immune to varicella. Therefore, even if a person does not recall having chickenpox, serologic testing for varicella immunity is not recommended. It is often a barrier to herpes zoster vaccination, and false negatives are common. However, if serologic evidence of varicella susceptibility becomes available to the healthcare provider, providers should follow ACIP guidelines for varicella vaccination. Shingrix has not been evaluated in persons who are seronegative to varicella, and it is not indicated for the prevention of varicella.
For adults 19 years of age and older who are or will be immunocompromised, see .
Clinical Herpes Simplex Infection
Primary infection with herpes simplex involves grouped vesicles on an erythematous base. Mucocutaneus manifestations include eczema herpeticum, herpetic whitlow, herpes gladiatorum, folliculitis, or a severe/chronic mucocutaneous infection. Extracutaneous manifestations include ocular HSV keratoconjunctivitis. Herpes Encephalitis, Proctitis, and Neonatal HSV. These manifestations are often the ones with prominent morbidity and mortality .
Ocular HSV infection has complications that include corneal ulceration and scarring, globe rupture, and subsequent blindness. Epithelial keratitis has strong links to viral replication, while stromal keratitis is primarily immunopathologic and is promoted mainly by T cells . Consequently, HSV is one of the main causes of infectious blindness in developed countries .
Herpes encephalitis has > 70% mortality without treatment, with residual neurological defects in most surviving patients . Similarly, disseminated neonatal HSV has 50% mortality without treatment, 15% with treatment and with neurologic deficits in many recovering patients .
Read Also: Does Washing Hands Kill Herpes Virus
Read Also: How To Eliminate Herpes Forever
Do Condoms Help Prevent The Spread Of Genital Herpes
Yes. To prevent transmission of herpes, we recommend that condoms be used 100% of the time. Many patients will shed the virus and be contagious when they dont have symptoms. Studies have shown that asymptomatic shedding occurs between 1% and 3% of the time in patients with HSV II genital infections. Many new herpes infections occur from partners who are shedding the virus asymptomatically, so condoms are highly recommended.
Condoms may not be an attractive option for monogamous couples or for couples who desire to become pregnant. Couples may opt to have serological tests to determine if either partner has an asymptomatic infection. In close monogamous relationships, the risks of transmission can be weighed against other relationship issues, such as intimacy and pregnancy.
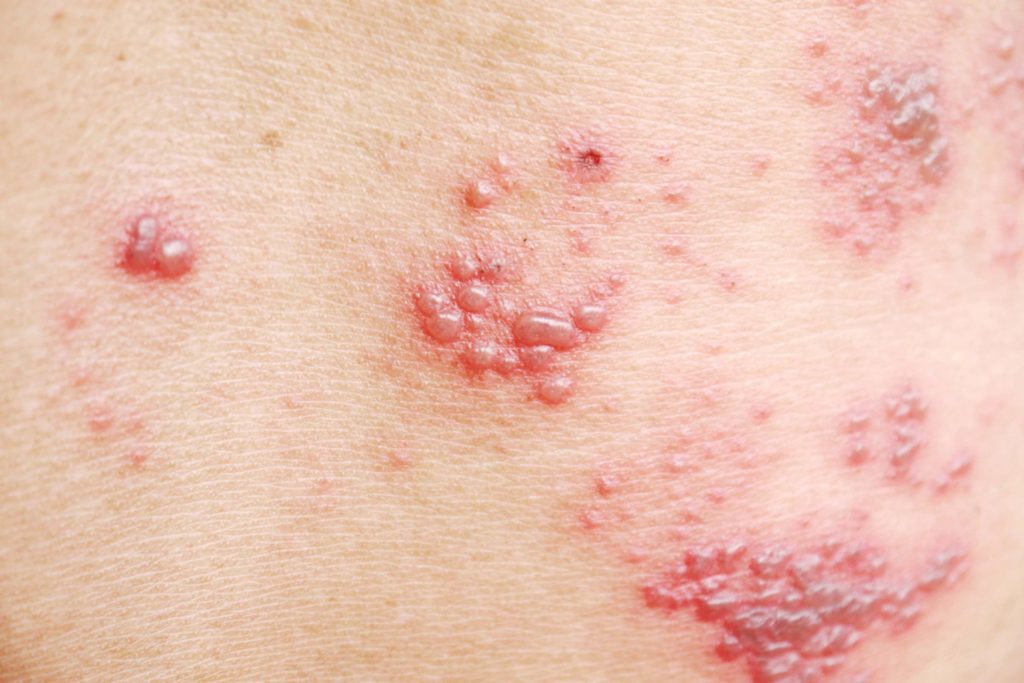
What Does Genital Herpes Look Like
While some people with genital herpes will never have any symptoms, other people can develop symptoms within a few weeks of being infected.
Often, before the lesions appear, patients describe a prodrome, characterized by a tingling or burning sensation in the area where the lesions will develop that can be noticed during urination, along with itching or discomfort in the genital area.
You can also have the following symptoms:
- Blisters on the mouth or lips
- Fever, headache or pain in the joints
- Trouble urinating
The symptoms of genital herpes often go away and come back as recurring outbreaks. For most people, the first outbreak is the worst, and can last from two to three weeks. Future flare-ups are often less severe and do not last as long. Still, some people shed the virus regularly. The following triggers can make outbreaks more likely to occur:
- Viral or bacterial infections
- Menstrual periods
Recurrent genital herpes is most common in the first year after the initial infection and decreases as time goes on.
In many cases, anti-herpes medicine can help patients. When a person experiences a prodrome and suspects a recurrence is going to happen, they begin taking anti-herpes medications that lessen symptoms and shorten the time of the outbreak.
Don’t Miss: What To Put On Herpes Sores
Routine Vaccination Of People 50 Years Old And Older
CDC recommends Shingrix for the prevention of herpes zoster and related complications. CDC recommends two doses of Shingrix separated by 2 to 6 months for immunocompetent adults aged 50 years and older:
- Whether or not they report a prior episode of herpes zoster.
- Whether or not they report a prior dose of Zostavax, a shingles vaccine that is no longer available for use in the United States.
- It is not necessary to screen, either verbally or by laboratory serology, for evidence of prior varicella.
Recombinant and adjuvanted vaccines, such as Shingrix, can be administered concomitantly, at different anatomic sites, with other adult vaccines, including COVID-19 vaccines. Coadministration of RZV with adjuvanted influenza vaccine and COVID-19 vaccines is being studied.
Replication Defective Virus Vaccine
Dl5-29 is a strain of HSV-2 with mutations in essential viral genes UL5 and UL29 making it replication defective. It was tested as both a prophylactic and therapeutic vaccine. It was shown to be safe, producing neutralizing antibodies and CD4+ T-cell responses in seronegative subjects who were vaccinated . Recent studies have demonstrated the production of antibodies mediating NK cell activation. Additionally, HSV-2 gD antibodies were detected in cervicovaginal fluid at around one-third of the serum level .
Recommended Reading: How To Stop Herpes Burning
What Are The Complications Of Shingles
After the shingles rash has disappeared, you might continue to have nerve pain in that same area. Postherpetic neuralgia can last for months or years and become quite severe.
More than 10% of people who get shingles develop postherpetic neuralgia. Researchers dont know why some people get postherpetic neuralgia and others dont. It may be that nerves become more sensitive or that the virus may be invading and damaging the central nervous system.
Other complications include:
- Other types of nerve issues like numbness or itching.
- A bacterial infection of the shingles rash.
- Eye and ear inflammation if the rash is near these organs.
What Are The Possible Side Effects Of Shingrix

Studies show that Shingrix is safe. The vaccine helps your body create a strong defense against shingles. As a result, you are likely to have temporary side effects from getting the shots. The side effects might affect your ability to do normal daily activities for 2 to 3 days.
Most people got a sore arm with mild or moderate pain after getting Shingrix, and some also had redness and swelling where they got the shot. Some people felt tired, had muscle pain, a headache, shivering, fever, stomach pain, or nausea. Some people who got Shingrix experienced side effects that prevented them from doing regular activities. Symptoms went away on their own in about 2 to 3 days. Side effects were more common in younger people.
You might have a reaction to the first or second dose of Shingrix, or both doses. If you experience side effects, you may choose to take over-the-counter pain medicine such as ibuprofen or acetaminophen.
Guillain-Barré syndrome , a serious nervous system disorder, has been reported very rarely after Shingrix. There is also a very small increased risk of GBS after having shingles.
If you experience side effects from Shingrix, you should report them to the Vaccine Adverse Event Reporting System . Your doctor might file this report, or you can do it yourself through the VAERS websiteexternal icon, or by calling 1-800-822-7967.
If you have any questions about side effects from Shingrix, talk with your doctor.
Read Also: Over The Counter Herpes Medication Walgreens