Exact Answer: Up To 10 Days
The herpes outbreak can stay for around one to two weeks. Some people with good health conditions would recover faster. There are many factors and conditions that would affect the lasting time of herpes. The type of herpes would cause a huge difference in the lasting time of herpes.
The lasting time of oral herpes would be different from genital herpes. The symptoms of herpes would come after a few days of virus exposure. There is no such specific treatment to treat the symptoms of herpes. The doctor may ask the patients to do certain hygiene care and treatment to get rid of a herpes outbreak.
How Long After Herpes Outbreak Is It Still Contagious
For oral herpes, cold sores are usually contagious for up to 15 days and are generally no longer contagious once all symptoms have cleared, which includes the blister itself and any scabbing.
Someone carrying genital herpes should wait until 7 days after the sore heals to begin engaging in sexual activity, as the herpes virus can spread from sores not covered by a condom.
Do Natural Remedies Help
There are several options that can be tried to ease the pain. A73612 and Donnor52059 suggest dabbing cornstarch directly on the sores. I can’t find any scientific studies that have researched this, but I can’t see that it would do any harm.
A73612 also recommends squirting water from a bottle over the sores when you pee. This is a time-honoured method that will help to ease the pain.
Yolandayw mentioned taking a simple painkiller such as paracetamol during an outbreak. Feelbroken advised putting Vaseline on the sores. Lidocaine 5%, a local anaesthetic gel that numbs the area, is another option. Some people find it helpful to put on five minutes before passing urine. You need to get it on prescription and it doesn’t suit everyone. Some people develop sensitivity to it which makes the symptoms worse.
Yolandayw also advised using ice as a home remedy. Simply wrap the ice in a tea towel and apply for 5-10 minutes. Never put ice directly on the skin as this can cause ‘ice burn’. Drinking plenty of water can also be helpful as it reduces the concentration of urine, making it less painful when you have to pee.
D91907 mentioned putting aloe vera gel on the sores. There is some scientific evidence that aloe vera is useful for both genital and oral herpes.
Read Also: Is Hpv The Same As Herpes
How To Cope After Diagnosis
Many posters were occupied with the issue of passing on the infection. Yolandayw points out that you can minimise the risk of transmission by postponing sex until all the sores have healed. She also mentioned that condoms should be used. They won’t completely prevent transmission but they will help.
Ending on a positive note, many posters emphasised that there was light at the end of the tunnel. Learning of the diagnosis may feel stressful at first, but it’s a manageable condition and certainly nothing to be ashamed of. Lucy03934 has had genital herpes for 25 years. She’s been married for 18 years and has two sons – living proof that there is life after herpes.
Can I Treat Herpes Simplex At Home
Avoiding known triggers, such as illness or stress, can help reduce how often you have herpes outbreaks.
How can I ease my symptoms during an outbreak of HSV-1 ?
- Over-the-counter creams such as L-lysine, benzocaine or docosanol .
- Applying ice to blisters or sores.
How can I ease my symptoms during an outbreak of HSV-2 ?
- Apply an ice pack to your genitals. Wrap the ice pack in a washcloth or apply it over your underwear.
- Keep your genitals dry. Wear cotton or other nonsynthetic underpants and avoid tight-fitting clothes. Moist sores take longer to heal.
- Soak in a warm bath.
- Take nonsteroidal anti-inflammatory drugs to relieve pain.
- Topical 1% or 2% lidocaine may be used as a topical analgesic.
You May Like: Does Genital Herpes Cure Itself
How Can I Prevent Herpes Outbreaks
If you have lots of herpes outbreaks, your doctor may tell you to take medicine every day this is called suppressive therapy. It can help prevent future herpes outbreaks, and lower your chances of giving herpes to your partners.
Whether or not you take medicine to treat herpes, taking care of yourself by eating healthy foods, getting enough sleep, and avoiding stress might help keep future outbreaks from popping up.
No one knows for sure what triggers genital herpes outbreaks. Other infections, surgery, sex, your period, skin irritations, and stress may cause outbreaks. Sunburns, injuries to your lips, or other infections can cause oral herpes flare-ups. Try to avoid getting sunburned if you have oral herpes.
Genital herpes outbreaks usually happen less often and become shorter and weaker after a few years whether or not you get treated.
Why People Are Talking About Covid And Herpes
First, letâs talk about how the COVID vaccine became linked to herpes in the first place.
A recent study published in Rheumatologylooked at the effect of mRNA-based vaccines on patients with autoimmune inflammatory rheumatic diseases â a group of diseases that cause your immune system to attack your joints, muscles, bones, and organs, such as rheumatoid arthritis, systemic lupus erythematosus, Sjögren syndrome, and polymyositis.
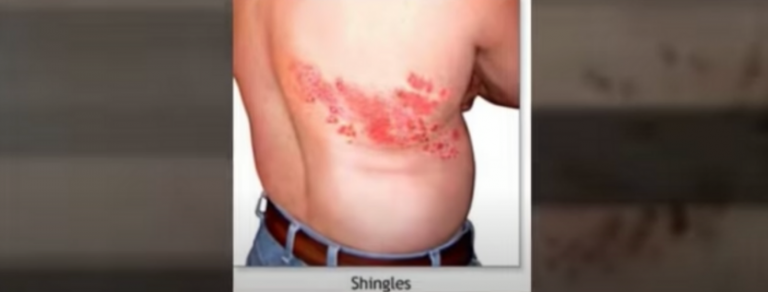
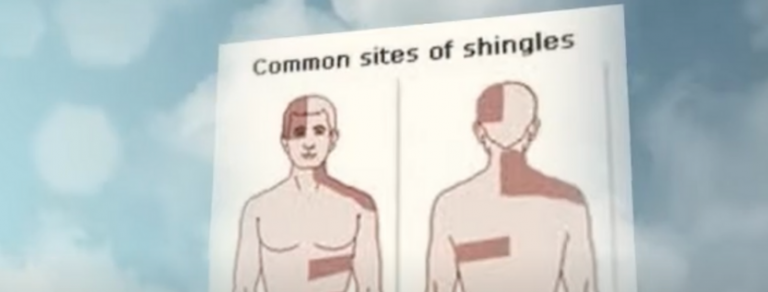
The study reported that out of 491 patients with AIIRD, six adult women developed herpes zoster infections, aka shingles, within three to 14 days after receiving the Pfizer vaccine â five developed symptoms after their first dose and one after receiving the second dose. The researchers noted that these six women accounted for only 1.2 percent of the 491 patients with AIIRD involved in the study. Meanwhile, zero patients in the control group experienced a herpes zoster infection after vaccination.
The information was then published on April 20 in the New York Post, where it began making the rounds online. And though the studyâs lead author, Victoria Furer, M.D., did tell the Jerusalem Postthat thereâs no causal link between the two , she mentioned that the vaccine could be a âtriggerâ to patients with similar pre-existing conditions. And this was enough to create a little internet frenzy particularly among those who are already skeptical of getting the vaccine in the first place.
You May Like: How To Get Rid Of Herpes Around The Mouth
You May Like: How To Stop Herpes From Burning
If You Have Symptoms Find Out What Youre Dealing With
With genital herpes, the biggest mistake people make is not seeking medical advice, says Gade.
People often find the signs or symptoms of a first herpes outbreak confusing, says Gade. You may mistake herpes symptoms for those of a yeast infection and try curing that condition on your own. But if your healthcare provider diagnoses you with herpes, the first line of treatment will be antiviral medications.
, you can make matters worse by putting things on the herpes sores that you shouldnt put on the sores, she says. People often try using Vaseline, bacitracin, or Aquaphor to soothe the itchy or painful eruptions.
Honestly, not putting anything on the sores is best, says Gade. Do keep the area clean and dry, though.
Warm compresses applied to tender or painful areas can help. So can sitting in a warm bath, using Epsom salt.
Sometimes people have enormous pain with urination, says Gade. For relief, you can urinate in your bathwater or while taking a shower to dilute the urine stream and lessen the sensation. You can also use warm water in a spray bottle to dilute the stream while youre urinating.
When To Call A Doctor
If you haven’t been diagnosed with genital herpes, call your doctor if you have:
- Painful blisters or sores in the genital or pelvic area.
- Burning or pain while urinating, or you can’t urinate.
- Reason to think you’ve been exposed to genital herpes.
If you have been diagnosed with genital herpes, call your doctor if you are having frequent outbreaks or if you can’t pass urine or are constipated.
If you are pregnant and have genital herpes, or if you think you have genital herpes, tell your doctor.
Also Check: Do Herpes Outbreaks Happen In The Same Spot
Sexuality In Midlife And Beyond
The physical transformations the body undergoes with age have a major influence on sexuality. This Special Health Report, Sexuality in Midlife and Beyond, will take you through the stages of sexual response and explain how aging affects each. Youll also learn how chronic illnesses, common medications, and emotional issues can influence your sexual capabilities. Finally, youll find a detailed discussion of various medical treatments, counseling, and self-help techniques to address the most common types of sexual problems.
Get the latest in health news delivered to your inbox!
Thanks for visiting. Dont miss your FREE gift.
The Best Diets for Cognitive Fitness, is yours absolutely FREE when you sign up to receive Health Alerts from Harvard Medical School
Sign up to get tips for living a healthy lifestyle, with ways to fight inflammation and improve cognitive health, plus the latest advances in preventative medicine, diet and exercise, pain relief, blood pressure and cholesterol management, and more.
Health Alerts from Harvard Medical School
Get helpful tips and guidance for everything from fighting inflammation to finding the best diets for weight lossfrom exercises to build a stronger core to advice on treating cataracts. PLUS, the latest news on medical advances and breakthroughs from Harvard Medical School experts.
BONUS! Sign up now and get a FREE copy of theBest Diets for Cognitive Fitness
Stay on top of latest health news from Harvard Medical School.
Coping With Your Feelings
Finding out that you have genital herpes may cause you to have negative thoughts or feelings about yourself or about sex, such as:
- Feeling ashamed or embarrassed.
- Being afraid of the consequences of the infection.
- Being angry at the person who infected you.
- Feeling frustrated with treatment or recurrent outbreaks.
- Feeling scared to have sex.
A counselor or support groups for people with herpes may be helpful.
Read Also: How To Have Kids With Herpes
How Do I Talk With People About Having Herpes
It might feel scary to admit you have herpes, but talking about things can really ease your mind. You could lean on a close, non-judgmental friend that you trust to keep the conversation private. Parents, brothers and sisters, aunts and uncles, and other family members can also be a source of comfort. Remember, herpes is really common, so its possible the person youre talking to has herpes, too.
There are a lot of online support groups for people who have herpes, and the American Sexual Health Association has a list of support groups that meet in person.
Treatment If The Blisters Come Back
Go to a GP or sexual health clinic if you have been diagnosed with genital herpes and need treatment for an outbreak.
Antiviral medicine may help shorten an outbreak by 1 or 2 days if you start taking it as soon as symptoms appear.
But outbreaks usually settle by themselves, so you may not need treatment.
Recurrent outbreaks are usually milder than the first episode of genital herpes.
Over time, outbreaks tend to happen less often and be less severe. Some people never have outbreaks.
Some people who have more than 6 outbreaks in a year may benefit from taking antiviral medicine for 6 to 12 months.
If you still have outbreaks of genital herpes during this time, you may be referred to a specialist.
You May Like: How Do They Test For Herpes 2
How Does Genital Herpes Affect A Pregnant Woman And Her Baby
Neonatal herpes is one of the most serious complications of genital herpes.5,16 Healthcare providers should ask all pregnant women if they have a history of genital herpes.11 Herpes infection can be passed from mother to child during pregnancy or childbirth, or babies may be infected shortly after birth, resulting in a potentially fatal neonatal herpes infection. 17 Infants born to women who acquire genital herpes close to the time of delivery and are shedding virus at delivery are at a much higher risk for developing neonatal herpes, compared with women who have recurrent genital herpes . 16,18-20 Thus, it is important that women avoid contracting herpes during pregnancy. Women should be counseled to abstain from intercourse during the third trimester with partners known to have or suspected of having genital herpes. 5,11
Recommended Reading: What Are The Side Effects Of Herpes
Sex And Physical Irritation
Friction from intercourse can irritate tissue and trigger a herpes outbreak.
Obviously, that doesnt mean to avoid having sex forever or that youll break out if you do.
But it does mean if youre having early warning signs that an outbreak is coming on, like sensitivity or tingling, then wait for them to pass.
They may be prodrome symptoms that signal contagiousness and an impending outbreak. And making them worse might encourage the outbreak to happen.
So since sex can sometimes trigger outbreaks, just be careful to minimize irritation. Try using a water-based lubricant. However, lubricants that contain the spermicide nonoxynol-9 can irritate soft tissue of the vaginal walls.
Other physical irritations can cause herpes outbreaks:
Also Check: How Are You Tested For Herpes
What Are The Signs Of Herpes In Women
Like men, women who have HSV-1 or HSV-2 may have no symptoms or signs of the infection. Some women may only have an initial outbreak and no other recurring symptoms. Others may have chronic recurring outbreaks of the herpes virus, and some women may not have an outbreak for months or even years after they have first been infected.
In the first herpes outbreak, symptoms usually start within 2 weeks of contracting the virus. The initial symptoms may include:
-Headache
-Around the buttocks or thighs
-Inside the cervix or urinary tract
How Often Do Outbreaks Occur
The number of outbreaks someone has varies from person to person. The average number of outbreaks for a person with genital HSV-2 is four to five per year. The average for genital HSV-1 is less than one outbreak per year.
Usually, there are more outbreaks during the first year, and many people find that outbreaks become less severe and less frequent with time.
Herpes triggers are highly individual, but with time, many people learn to recognize, and sometimes avoid, factors that seem to reactivate HSV in their own bodies. Illness, poor diet, emotional or physical stress, friction in the genital area, prolonged exposure to ultraviolet light , surgical trauma, and steroidal medication may trigger a herpes outbreak.
The frequency of outbreaks can often be managed through effective stress management, and getting adequate rest, nutrition, and exercise. For people with frequent outbreaks, suppressive therapy with any one of the antiviral treatments can reduce outbreaks by as much as 80%.
You May Like: No Herpes Outbreak In Years
Who Might Get Herpes Simplex
People of any age can contract herpes simplex. You are more likely to get the virus if you:
- Were assigned female at birth.
- Have had multiple sex partners.
- Started having sex at a young age.
- Have a history of any sexually transmitted infection .
- Have a weakened immune system.
- Dont use condoms for intercourse and dental dams for oral sex.
Who gets HSV-1, commonly known as oral herpes?
Anyone can get HSV-1. Most people contract HSV-1 during childhood. It spreads when an adult who has the virus has close contact with a child, such as when a family member kisses a child.
Who gets HSV-2, commonly known as genital herpes?
Genital herpes affects sexually active teens and adults of all genders and races. It can spread if you have multiple sexual partners and dont use condoms or dental dams.
People assigned female at birth are more at risk. Delicate vaginal tissue can tear, making it easier for the infection to get in. Black people who were AFAB are especially vulnerable, with an estimated 1 in 2 people AFAB between the ages of 14 and 49 infected with HSV-2.
Treatment Of Recurrent Infection
Recurrences of herpes are often mild and infrequent, and most patients do not seek treatment. Drug therapy to prevent recurrences is available and effective, but because of cost and inconvenience issues, it is traditionally reserved for use in patients who have more than six outbreaks per year. Suppressive therapy in these patients is intended to reduce the frequency and severity of herpes symptoms, decrease the transmission of HSV to sexual partners and infants of infected mothers, and decrease the transmission of associated viral diseases . Unfortunately, only the first goal has yet proved to be attainable.
Acyclovir has been used to suppress recurrences of genital herpes, decreasing the frequency by as much as 80 percent and preventing recurrence by as much as 45 percent of patients.6 Successful suppression for as long as five years without adverse effects has been reported.3 The drug is titrated from a starting dose of 400 mg twice daily to achieve maximal efficacy with the lowest, least frequent dose.1 Therapy should be discontinued once a year to assess whether its continuation is necessary. In addition, cost and compliance should be discussed with the patient. Acyclovir resistance has not been a problem in immunocompetent patients but has been documented in 4 percent of HIV-infected persons.1
Dosages and Characteristics of Chronic Suppressive Treatment Regimens for Recurrent Genital Herpes Infection
This dosage is not FDA-labeled for this indication.
Read Also: What Are Genital Herpes Pictures
How Can Herpes Be Prevented
Correct and consistent use of latex condoms can reduce, but not eliminate, the risk of transmitting or acquiring genital herpes because herpes virus shedding can occur in areas that are not covered by a condom.25,26
The surest way to avoid transmission of STDs, including genital herpes, is to abstain from sexual contact, or to be in a long-term mutually monogamous relationship with a partner who has been tested for STDs and is known to be uninfected.
Persons with herpes should abstain from sexual activity with partners when herpes lesions or other symptoms of herpes are present. It is important to know that even if a person does not have any symptoms, he or she can still infect sex partners. Sex partners of infected persons should be advised that they may become infected and they should use condoms to reduce the risk. Sex partners can seek testing to determine if they are infected with HSV.
Daily treatment with valacyclovir decreases the rate of HSV-2 transmission in discordant, heterosexual couples in which the source partner has a history of genital HSV-2 infection. 27 Such couples should be encouraged to consider suppressive antiviral therapy as part of a strategy to prevent transmission, in addition to consistent condom use and avoidance of sexual activity during recurrences.
6 likes, 110 replies